
Has your baby been experiencing breathing issues, and has your doctor recommended a pulmonary function test? For many parents, hearing that an infant may need specialized lung testing can feel overwhelming. Pulmonary concerns in babies are stressful, especially when symptoms like wheezing, labored breathing, or repeated infections don’t seem to improve. Understanding how pulmonary function tests work for infants and why they are recommended can help parents feel informed, prepared, and confident in the care their child is receiving.
This guide explains current guidelines and techniques for infant pulmonary function testing, why these tests differ from those used in older children, and what parents can expect before, during, and after the evaluation.
What Is a Pulmonary Function Test for Infants?
A pulmonary function test evaluates how well the lungs move air in and out and how effectively oxygen is delivered throughout the body. In infants, this type of testing is often referred to as infant pulmonary function testing (iPFT).
Because babies cannot follow instructions like “take a deep breath and blow,” infant testing relies on passive, highly specialized methods performed while the baby is asleep or lightly sedated. These evaluations are conducted under strict ATS/ERS standards for infants, developed by the ERS/ATS task force, to ensure safety, accuracy, and comfort.
Unlike spirometry used in older children, infant pulmonary testing focuses on measuring breathing mechanics rather than effort-based breathing.
When Pulmonary Function Testing Is Recommended for Infants
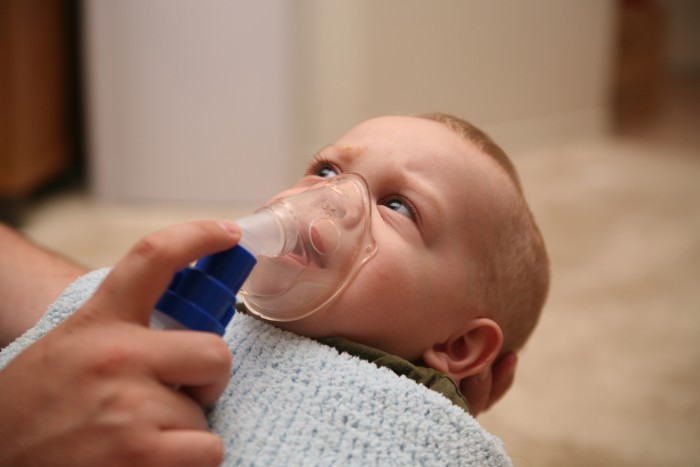
Pediatric pulmonologists do not recommend infant pulmonary function tests casually. These evaluations are typically ordered when a baby shows persistent or concerning respiratory symptoms that cannot be fully explained through routine exams.
Common clinical indicators include:
- Persistent wheezing in infants that does not respond to standard treatment
- Recurrent respiratory infections, especially lower airway infections
- Increased breathing effort, such as visible chest movement or nasal flaring
- Respiratory retractions, where the skin pulls in around the ribs or neck
- Low oxygen saturation or episodes of hypoxemia in babies
- Ongoing infant respiratory distress without a clear diagnosis
Testing may also be used to evaluate known or suspected conditions such as bronchopulmonary dysplasia, cystic fibrosis, chronic lung disease in infants, or early signs of airway obstruction in infants.
How Infant Pulmonary Function Testing Differs from Spirometry

Many parents are familiar with spirometry, which requires active cooperation. However, spirometry is not suitable for newborns or young infants.
Infant testing relies on techniques designed specifically for non-cooperative infants, allowing clinicians to gather meaningful lung data without requiring effort from the baby.
Key differences include:
- Infants are tested while asleep rather than awake
- Breathing is measured passively using external equipment
- Results focus on lung mechanics and airflow patterns rather than voluntary effort
This distinction is why spirometry vs infant PFT comparisons matter when deciding the right test for a child’s age and developmental stage.
Core Techniques Used in Infant Pulmonary Function Testing
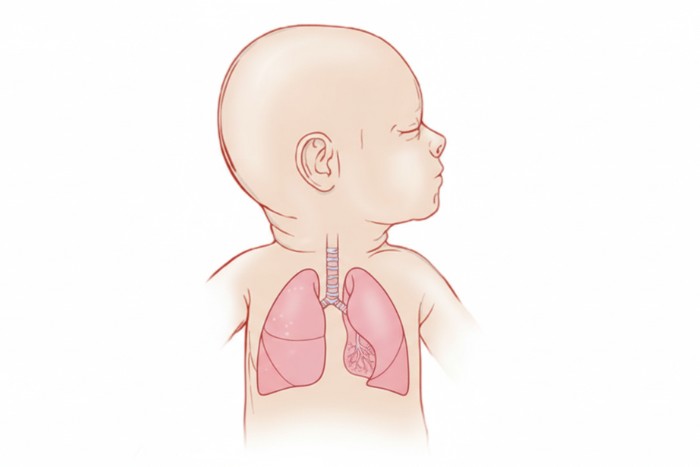
Rapid Thoracoabdominal Compression (RTC)
Rapid thoracoabdominal compression (RTC) uses gentle pressure applied to the chest and abdomen during exhalation to assess airflow limitation. A soft pneumatic vest is often used to deliver controlled compression.
Raised Volume RTC (RVRTC)
Raised volume RTC (RVRTC) expands on standard RTC by inflating the lungs to a set volume before compression. This method provides more detailed insight into airflow limitation and early airway obstruction in infants.
Tidal Breathing Flow-Volume Loops
Tidal breathing flow-volume loops (TBFVL) measure natural breathing patterns while the infant rests. These loops help identify abnormalities in airflow and breathing rhythm without forced maneuvers.
Functional Residual Capacity and Lung Volumes
Measurements such as functional residual capacity (FRC) and VmaxFRC assess how much air remains in the lungs after normal breathing. Techniques like body plethysmography and other lung volume measurement methods help evaluate lung size and elasticity.
Additional Advanced Methods
Some centers may also use:
- Passive lung inflation
- Thoracic compression techniques
- Impulse oscillometry (IOS) or forced oscillation technique (FOT) for specialized cases
All methods rely on carefully calibrated infant lung function equipment designed for newborn anatomy.
Sedation and Safety During Infant Pulmonary Function Tests

Because infants must remain still for reliable results, infant PFT sedation is commonly used. Light sedation allows the baby to sleep naturally during testing.
Common safety practices include:
- Use of medications such as chloral hydrate sedation when appropriate
- Pre-test vital signs screening
- Continuous pulse oximetry monitoring throughout the procedure
- Strict adherence to safety protocols for iPFT
Parents are often asked to follow a sleep deprivation protocol or fasting instructions for infants, including guidance on clear liquids pre-test, to ensure sedation is safe and effective.
Preparing Your Baby for a Pulmonary Function Test

Preparation plays a key role in test success. Families are usually given detailed instructions before the appointment.
Typical preparation steps include:
- Following fasting or feeding guidelines
- Adjusting nap schedules for sleep deprivation is recommended
- Bringing comfort items such as a blanket or pacifier
- Completing consent forms and medical history paperwork
Understanding preparation for baby PFT helps reduce stress and ensures the visit goes smoothly.
What Happens During the Visit

On the day of testing, families can expect:
- A check-in and review of medical history
- Placement of monitors for heart rate and oxygen levels
- Gentle positioning of the infant for testing
- Testing performed while the baby sleeps
- Close observation by trained clinical staff throughout
The environment is calm and controlled, with a strong focus on infant comfort and safety.
Interpreting Infant Pulmonary Function Test Results

After testing, results are reviewed by a pediatric pulmonologist with expertise in iPFT results interpretation. Findings help determine whether a baby shows signs of:
- Early respiratory disease
- Obstructive or restrictive breathing patterns
- Reduced lung volumes or abnormal airflow
Results often guide decisions about medications, inhaled therapies, oxygen support, or additional diagnostics such as imaging or bronchoscopy.
How Results Influence Treatment and Monitoring

Pulmonary function testing allows clinicians to move from observation to action. Based on results, a care plan may include:
- Adjustments to respiratory medications
- Monitoring strategies for infant asthma evaluation
- Referrals for pediatric pulmonologist care
- Long-term tracking of neonatal lung function
Early testing supports early intervention for respiratory conditions, helping protect lung development during critical growth periods.
Why Early Testing Matters

Infant lungs continue to develop rapidly during the first years of life. Identifying problems early allows providers to:
- Prevent progression of lung disease
- Improve breathing efficiency
- Reduce hospitalizations
- Support healthy growth and development
For parents, testing provides clarity and reassurance when symptoms are persistent or unclear.
Bringing It All Together
A pulmonary function test for infants is a highly specialized, carefully controlled evaluation designed to answer important questions about a baby’s breathing health. While the idea of lung testing in infancy can feel intimidating, these tests are guided by established ATS/ERS standards, performed with advanced safety measures, and interpreted by experts trained in infant respiratory care.
When symptoms such as wheezing, retractions, or low oxygen levels persist, infant pulmonary function testing offers valuable insight that helps clinicians create effective, individualized care plans.
If your pediatrician has suggested further respiratory evaluation or you have ongoing concerns about your baby’s breathing, early assessment can make a meaningful difference.
To learn more about infant pulmonary evaluations or to discuss whether testing may be appropriate for your child, contact Pediatric Associates of Dallas today.
